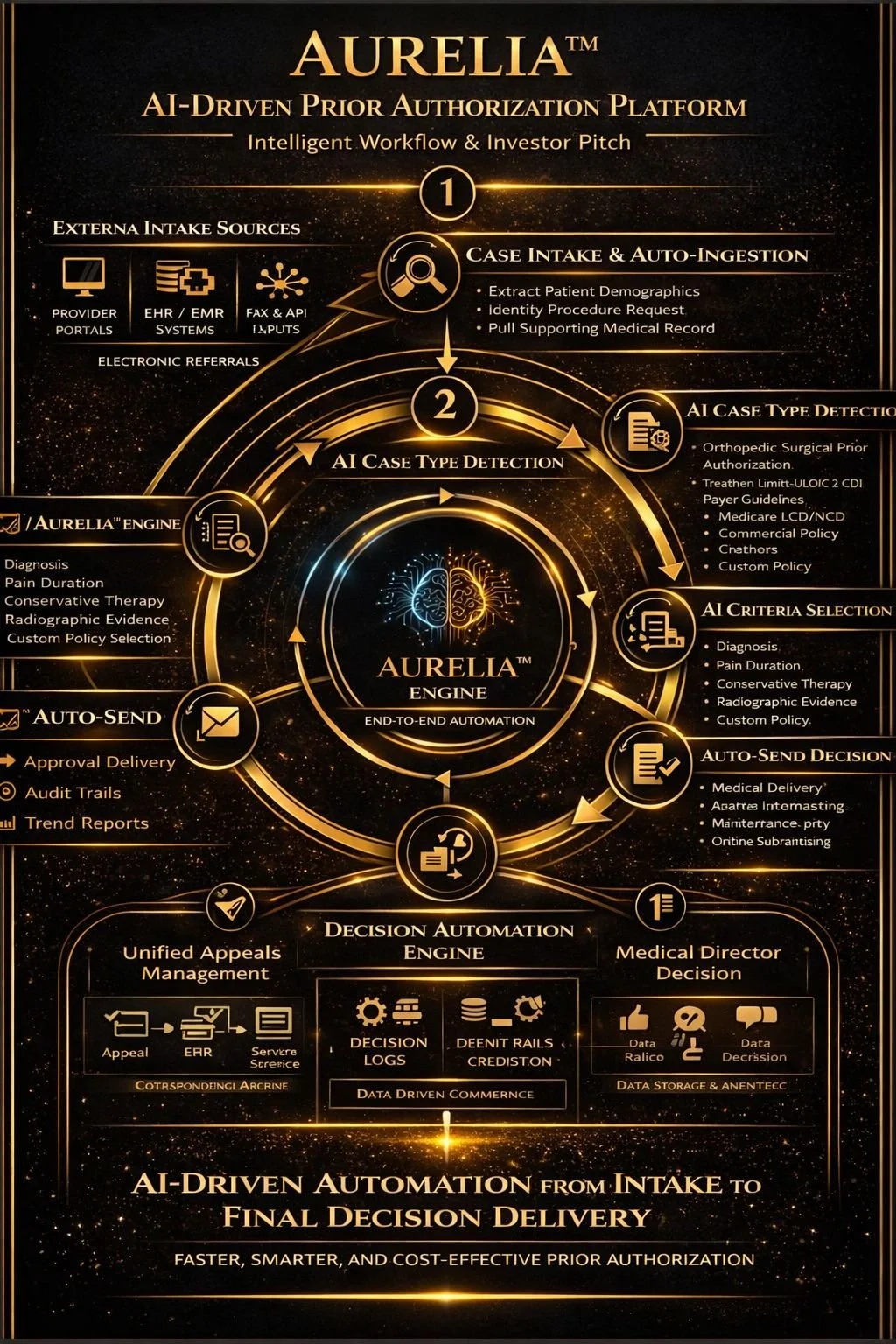
Explore our all-in-one Prior Authorization system workflow.
Aurelia: AI-Driven Prior Authorization Platform
Aurelia revolutionizes the prior authorization process by combining cutting-edge artificial intelligence with clinician-informed workflows. Designed to streamline approvals, reduce administrative burden, and optimize revenue cycle management, Aurelia empowers healthcare teams to work smarter, faster, and more efficiently.
With Aurelia, healthcare organizations can:
Automate Prior Authorizations: AI intelligently reviews patient data, identifies required authorizations, and initiates submissions with accuracy and speed.
Reduce Denials & Delays: By proactively detecting documentation gaps and payer-specific requirements, Aurelia minimizes claim denials and accelerates approvals.
Enhance Clinical Workflows: Seamlessly integrated with existing EHR systems, Aurelia reduces redundant tasks, freeing clinicians to focus on patient care.
Data-Driven Insights: Gain actionable analytics on approval trends, workflow bottlenecks, and utilization patterns to improve decision-making and operational efficiency.
Scalable & Adaptive: Aurelia adapts to different specialties, payer rules, and institutional workflows, making it a versatile solution for hospitals, clinics, and managed care organizations.
Built by experts in clinical documentation, utilization management, and revenue cycle operations, Aurelia bridges the gap between clinical intent and payer requirements, ensuring compliance while maximizing efficiency.
Aurelia doesn’t just automate—it transforms the prior authorization process into a seamless, intelligent system that supports both clinicians and administrators, improves patient access to care, and strengthens organizational performance.
Empower your team. Accelerate approvals. Redefine efficiency. With Aurelia, prior authorization has never been smarter.